Contents |
Glaucoma
Introduction
Glaucoma is a condition usually characterized by increased pressure of the fluid within the eyeball, which causes damage to the retinal nerve fibers and the optic nerve if left untreated. Pressure within the eyeball is measured in mm Hg, the same unit used to describe barometric pressure in weather prediction. The normal range of pressure within the eye is between about 12 mm Hg to 22 mm Hg.
In any discussion about glaucoma, a word that often gets used is “angle.” The fluids within the eye drain away into a sponge-like structure called the trabecular meshwork or trabeculum. This structure is located in the angle formed between the back of the cornea and the base of the iris. It is located inside the eye, just under the area where the clear cornea becomes white to form the sclera, the tough, connective-tissue outer covering of the eye. The trabeculum is more accessible with a wider angle, while a narrow angle makes drainage more difficult. The two major types of glaucoma are, in fact, described by the state of the angle in an individual’s eye. (Figure 1)
There are two general types of glaucoma, called "primary open-angle glaucoma (POAG)" and "Angle-Closure Glaucoma (ACG)", which present in very different ways and are usually thought of by clinicians as being two separate diseases.
ACG is the rarer of the two types, accounting for about 10% of all glaucoma cases. This type of glaucoma presents as a rapid increase in "intraocular pressure (IOP)" which causes pain, headache, blurred vision and halos around lights. People who are farsighted (hyperopic) and are of Asian descent are more likely to experience acute episodes of ACG, which can occur spontaneously, or may be triggered by the pupil dilating, as it would in a dark theatre, or while driving at night, for instance.
"Angle-closure glaucoma is a sight-threatening emergency" and must be treated as soon as possible to reduce the pressure within the eye before permanent vision loss occurs. For more information about this particular type of glaucoma, please see our article titled Angle-Closure Glaucoma.
Primary Open-Angle Glaucoma, or POAG, is much more common, comprising about 90% of all cases of glaucoma. This article will describe POAG, but if you think you may have had episodes of angle-closure glaucoma, see an eyecare practitioner right away for testing and treatment to prevent damage to your vision.
Causes of Glaucoma
Clinicians have long noted that glaucoma tends to run in families, so there is a definite hereditary factor at work; it is not, however, as simple as inheriting blue or brown eyes. If there is a family member with the disease, this is an important risk factor.
Another risk factor for POAG is simply age; as we age, the crystalline lens within the eye becomes thicker, pushing the iris further forward and possibly causing drainage from the angle to slow and allows IOP to rise.
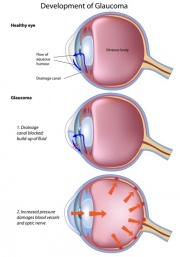
Normally, the fluids within the eye are constantly being replenished as they drain away. Cells lining the ciliary body (diagram) are constantly producing aqueous humour, which circulates into the anterior chamber between the cornea and the iris, where it drains out through a sponge-like tissue called the "trabecular meshwork" located in the "angle" formed by the cornea and the iris. [diagram] Ideally, the aqueous humour is being made at the same rate as it drains away, keeping the IOP steady and within the normal range.
However, sometimes the drainage mechanism in the angle begins to lose efficiency and leads to a gradual buildup of pressure within the eye, leading to glaucoma.
Some glaucoma cases are caused by the release of pigment from the iris as a result of inflammation or trauma; the pigment granules get caught in the drainage meshwork and impede the outflow of aqueous.
If you think of the eye as if it were a sink with a continually dripping faucet, you can visualize what would happen if the drain were to slowly clog up; gradually, the fluid dripping into the sink will build up until it overflows. In glaucoma, the eyeball cannot overflow, so the pressure within it rises.
When the pressure inside a balloon becomes too high, the balloon pops, but the eye is made of very strong connective tissue called the "sclera", which does not burst; instead, the increased pressure within the eye begins to compress the weakest area, the head of the optic nerve. Over a million retinal nerve fibers come together there to carry visual information to the brain; increased pressure within the eye compresses the fibers, causing them to be damaged and, eventually, to die. The result of this damage is permanent vision loss.
Risk factors for glaucoma include:
- High myopia (nearsightedness)
- High hyperopia (farsightedness)
- Shallow anterior chamber on examination
- Regular long-term steroid use
- Previous eye injury
- Age over 45 years
- Any family history of any type of glaucoma
- Diabetes
- African descent
People who have one or more of these risk factors should have yearly eye examinations.
Symptoms and Signs
Unfortunately, POAG has no symptoms for an individual to be aware that there is a problem, until vision loss is quite extensive. Vision loss from POAG begins in the peripheral vision, so most people are not aware that their field of view is gradually shrinking.
The clinical signs of glaucoma are elevated IOP, characteristic changes in the peripheral visual fields and damage to the nerve fiber layer of the retina, as well as certain changes to the head of the optic nerve where these fibers come together.
It is important to understand that these signs are not detectable without a vision examination by an eyecare practitioner; there are no outward signs of glaucoma that can be seen otherwise. It is not possible to tell if the pressure within the eyes is too high by touching them.
Vision loss from glaucoma is permanent, so early diagnosis and treatment is necessary to preserve eyesight.
Treatment
Treatment of glaucoma is aimed towards decreasing IOP, either medically or surgically.
Medications are available, usually in the form of eyedrops that cause either the production of aqueous to slow down, or to increase the rate of drainage through the trabecular meshwork; sometimes it is helpful to use a combination of these types of medications to maintain control of the IOP and keep it within normal levels.
If necessary, surgery may be performed to open the drainage area in the angles. Recently, this type of surgery has become safer and more effective with the use of lasers rather than traditional surgical techniques.
If the pressure within the eye can be maintained at a level tolerable to the eye, damage to the vision can usually be prevented, although there is a rare form of the condition known as low-pressure or low-tension glaucoma, where the IOP as measured would be considered well within the normal range but visual damage occurs regardless. Most clinicians try to reduce IOP as much as possible, but it is not known why the eyes of some people are more susceptible to damage from what would be normal pressure for others. It is possible that there are episodic increases in IOP that elude measurement, but this has not been proven.
Vision loss from glaucoma is largely preventable when it is diagnosed and treated early. The best strategy for doing so is to have regular eye examinations.